The COVID-19 pandemic currently devastating the globe has infected almost 7 million people in India, resulting in over 100,000 deaths. The figure is comparable to the official reported deaths caused by Tuberculosis (TB) in 2019. Despite TB being a preventable disease, this is a yearly phenomenon.
Big cities have seen the highest concentration of COVID-19 cases. A district-wise analysis conducted in July showed that a mere 10 cities (including Mumbai) accounted for 52.7% of all active cases in the country. The infection is more widespread now, but Mumbai continues to be among the worst hit cities. Its sprawling slum population, cramped dwellings, and high population density made it virtually impossible for many to “social distance” and presented itself as the optimal breeding ground for this highly infectious disease to spread.
As of 9th October 2020, Mumbai’s COVID-19 count stood at almost 260,000 positive cases, with a fatality rate of approximately 3.6%.
Apart from COVID-19, Mumbai suffers the burden of a highly concentrated TB epidemic, with an incidence rate of approximately 418 per 100,000 of population, and an appallingly high fatality rate of 11% (calculated based on Nikshay Portal resident ‘TB Notifications’ for Mumbai in 2018 compared to ‘TB Deaths’ registered for the same year by MCGM).
The advent of COVID-19, the many successive lockdowns, and the rapid changes in healthcare systems had a staggering impact on the provision of healthcare. Healthcare facilities were overburdened, and the already scarce number of healthcare personnel were redistributed and diverted to COVID-19 control services. Non COVID-19 essential health services bore the brunt of these rapid changes, and were subsequently neglected. A culmination of these factors led to a dramatic drop in both access to essential TB treatment and number of TB Notifications.
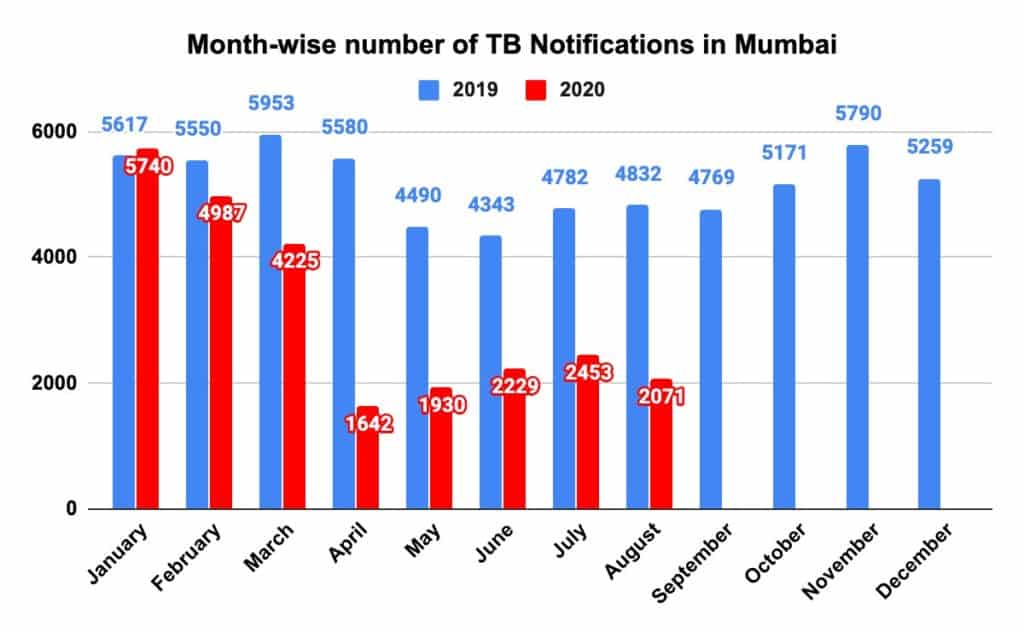
January 2020 had one of the highest notification rates (5,740) of any month from the previous years. However, April 2020 saw the number of notifications drop to 1,642, which was a shocking 71% lower than recorded in January 2020, and 63.5% less than what was recorded in April 2019.
TB Notifications are a particularly important tool in controlling the spread of the disease. Their purpose is to enable routine surveillance to pinpoint sources of outbreaks and areas with high TB burdens, and to provide access to timely and adequate treatment.
Treatment in the case of TB is doubly important as the improper or untimely administration of treatment leads to a more vitriolic form known as Drug-Resistant TB (DR-TB), which is resistant to a number of first and second line TB drugs.
Multi-Drug-Resistant TB (MDR-TB) is resistant to the two first-line drugs, rifampicin and isoniazid. Extensively-Drug-Resistant TB (XDR-TB) is resistant to rifampicin and isoniazid, plus any fluoroquinolone and one of the injectable second-line drugs (amikacin, capreomycin, or kanamycin).
The DR-TB strains do not respond to the standard TB treatments, but instead require aggressive interventions that involve a higher treatment time, cost, and come with a larger range of side effects. DR-TB can also be transmitted from person to person. Additionally treatments for DR-TB have a mere 47% success rate, in comparison with Drug-Sensitive TB, which has a 79% success rate, according to India TB Report 2019.
This has important implications not just for Mumbai, but for India as a whole. While the number of notifications in India rose by 60%, from 1.2 million to 2.7 million from 2013 to 2019, COVID-19 greatly affected this progress.
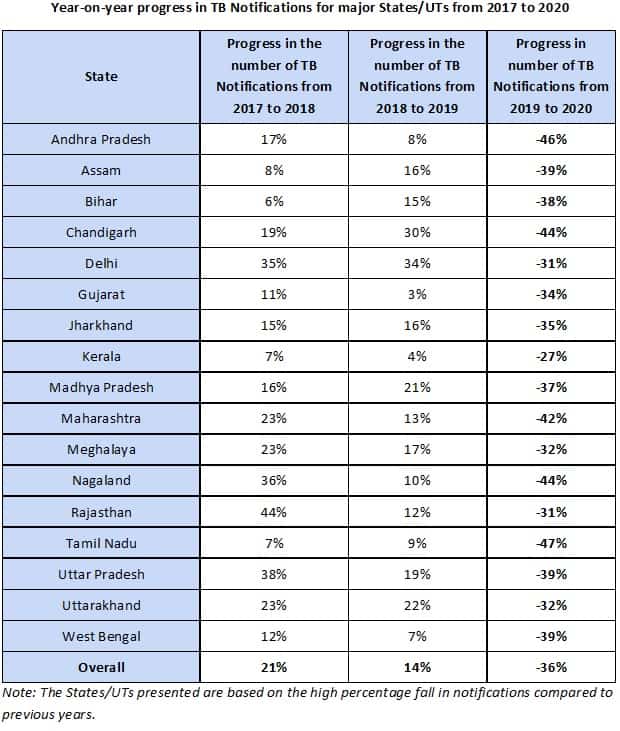
Overall, India saw a reduction of 36% in the number of TB Notifications, with the drop being as sharp as 47% in some states. This means that a much smaller number of possible TB carriers were accessing healthcare services, and receiving the necessary treatment. This has the dual unfavorable outcome of an increase in TB mortality, and simultaneous increase in the number of potential DR-TB carriers.
According to data available on the Public Health Portal of Municipal Corporation of Greater Mumbai (MCGM), the number of DR-TB (MDR-TB and XDR-TB) cases in Mumbai also appears to be at an all-time high, as of 2018.
Taking into consideration Mumbai’s heavy TB burden, rising DR-TB cases, and falling TB Notifications, a frightening scenario emerges. While preventive lockdown measures may have succeeded in lessening Mumbai’s COVID-19 burden to some extent, they greatly decelerated its TB programme; which until then appeared to have been making progress. Though lockdown restrictions have now lessened, TB Notifications have not increased proportionally. A reduction of TB control and treatment in a city like Mumbai could lead to a DR-TB epidemic, which would prove to be a catastrophic, financially infeasible, and socially disastrous predicament.
The United Nations Sustainable Development Goals (SDGs) have set out a global target to eliminate TB by 2030. India has pledged to achieve this by 2025. In order to reach elimination status, we would have to reduce our TB incidence to less than 1 case per 100,000 people. As per the India TB Report 2020, our national TB incidence is estimated at 200 per 100,000 people. Considering this, attaining elimination status by 2025 is truly a herculean task. Mumbai, with a TB incidence of 418 cases per 100,000 people has a paramount role to play in this battle towards a “TB Free India”.
While maintaining COVID-19 control efforts and preventing more deaths are of the utmost importance, they cannot be shouldered at the cost of other essential health services.
Data accessed from MCGM indicates that 64,349 deaths had taken place in Mumbai from January to July 2020, as against 51,972 for the same period in 2019. This excess of deaths is not due to COVID-19 alone, which only makes up for 10% of the total (6,530 COVID-19 deaths as on 31st July 2020). This clearly indicates that 90% of the deaths and the provision of other essential medical services, including TB are being neglected.
In a precarious situation like this, a dual strategy for simultaneous COVID-19 and TB essential services is imperative to limit the spread of both these highly infectious diseases. This requires a concerted effort to mitigate the looming threat of a sharp spike in DR-TB cases and TB deaths to ensure that the controlling of a pandemic doesn’t lead to a subsequent epidemic. Additionally, in line with the National Health Policy 2017’s vision of “prevention first”, it is also of supreme importance that essential health services for other diseases continue uninterrupted. It is necessary to focus on averting not just COVID-19 deaths, but also preventable non-COVID-19 deaths.
All charts provided by the author.
Also read:
Lockdown realities: How parents are turning therapists for kids with cerebral palsy
COVID-19 has put the spotlight on mental health, but India needs more
Life finds a way: A complete guide for expectant mothers in the time of COVID-19